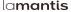In physiological conditions, a structure known as a follicle that contains an egg grows every month in each of the ovaries alternately. During ovulation, the ovary releases this egg, which is collected by the Fallopian tube, where, if possible, spermatozoa arrive to fertilise it.
Several mature and good-quality eggs are required to increase the effectiveness of IVF and achieve the pregnancy desired. Controlled ovarian stimulation, with hormonal treatment (gonadotropins), should therefore be performed for 9 to 12 days. This will allow for the growth of several follicles and, therefore, the retrieval of different eggs.
The stimulation protocol best suited to each patient is determined by the gynaecologist. During this period, strict personal and ultrasound scans are run to evaluate the number and growth of the follicles and hormone tests are performed.
When ovarian stimulation is deemed satisfactory, an HCG injection is administered. This allows for the final maturation of the eggs. Egg collection is scheduled for the subsequent 36 to 38 hours.